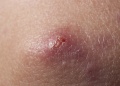
Boils or Furuncles
|
Boils or Furuncles | |
| Causes | Dietary Factors, Allergies, Infections, Prescription Medications, |
|---|---|
| See Also | Dermatology / Skin Conditions, Diabetes |
| Books | Books on Skin Diseases |
| Articles | Articles on Dermatology / Skin Conditions |
Boils, also called furuncles or abscesses, are a firm or fluctuant mass enclosing a collection of pus often due to an infection of the superficial folliculitis. [1]
Contents
Naturopathic Assessment
Causal Factors
In order to stimulate the innate ability of the body to heal the causes of disease must be identified and addressed. Boils are typically associated with infections yet there are other contributing factors that need to be considered.
Lifestyle
- Food allergies, nutrient deficiencies and excessive consumption of sugar (refined carbohydrates) are associated causes and can be an aggravating factor to cure [2].
| Check out this book | The Clear Skin Diet |
|---|
Social
- Emotional stress can be a trigger for boils, especially if someone is immune compromised.
Environmental
- Pathogens common with boils include Staphylococcus aureus, Escherichia coli, Pseudomonas aeruginosa, Streptococcus faecalis, Peptostreptococcus, Peptococcus, and Lactobacillus species.[1]
- Common infectious agents involved with boil formation include highly infective forms of bacteria like Staphylococcus aureus. [3]
- Previous infection with MRSA or methicillin-resistant Staphylococcus aureus and colonization is associated with repeated boils [2].
- Fungal infections on the skin's surface can cause boils.
- Other external risk factors for developing boils include HIV infection [2]
- Bartonella henselae causing cat-scratch disease can lead to abscess forming lyphadenopathy in children [4]
- Rectal colonization of Staph aureus versus nasal colonization in children is more often associated with soft-tissue abscesses/boils [5].
External
- Activities
- Contact sports such as wrestling and lacrosse are associated with boils [2].
- Drug Use
- Intravenous drug use is a risk factor for development of abscesses/boils [2].
Medical Interventions
- Prescription Medications
- MRSA or Methicillin resistant Staphylococcus aureus is becoming more prevalent and is associated with injection drug use, antibiotics, and admission to hospital in the previous year [6].
- Increasing use of vancomycin is occurring as a result of MRSA infection , as well as trimethoprim-sulfamethoxazole or clindamycin but growing concern over antibiotic resistance of these choices warrants consideration of more conservative and preventative management [6].
- Previous antibiotic therapy is a risk factor for boils.[7]
- Medical Treatments
- Previous hospitalization is a risk factor.[7]
Related Symptoms and Conditions
Conditions or diseases that may predispose a person to boils include:[3].
- Immune dysfunction
- Underlying bacteria infection
- Other skin diseases such as folliculitis
- Diabetes
- Obesity
- Malnutrition
- AIDS
- Cancer
Risk factors of recurrent furunculosis includes:[7]
- anemia
- previous antibiotic therapy
- diabetes mellitus
- previous hospitalization
- multiplicity of lesions
- personal hygiene
- associated skin diseases.
Characteristics
A boil often begins as a tender, pinkish-red swollen, firm area on the skin, but over time it can progress into a cyst that feels like a water-filled balloon.
- Pain is typically associated with the size of the boil. As the boil fills with pus and dead tissue the pain increases, as the boil drains the discomfort resolves.
- Boils may heal on their own, but often they require the boil to opened to assist with drainage.
- Characteristics of a boil include:
- Other symptoms associated with a boil can include:
Naturopathic Treatment
The goal of naturopathic treatment is to support and work in tandem with the healing power of the body and to address the causal factors of disease with individual treatment strategies. Boils are typically an acute disease. If boils are recurrent, last for longer than 2 weeks, are present on the spine or the middle of the face, or if they occur with a fever it is important to seek immediate medical care. The goal of treatment is to prevent any spread of infection and to support the natural healing process.
It is always advisable to work with a naturopathic doctor before engaging in any treatment plan.
Home Care
Home Care strategies include:
- The first step of any treatment plan is to maintain a diary of symptoms tracking diet, activity level, stress and other outside influences that may be triggering a flare-up.
- Ensuring proper hygiene of the area affected including regular hand washing, fomite cleaning, and avoiding contact with contaminated skin is required.[8]
- Warm, moist compresses help boils drain, which speeds healing. Gently soak the area (before the boil breaks and after) with a warm, moist cloth several times a day.
- Do not squeeze a boil or try to break it open at home as this can spread the infection and make it worse. The cutting of a boil is best done by a trained medical professional.
- Clean a draining boil often with clean cloths. Do not re-use or share washcloths or towels.
- Wash hands before and after touching the area around the boil.
- Wash all clothing, washcloths, towels or sheets that come into contact with the boil in hot water.
- Throw out all dressings in a tightly closed bag.
- Use only chemical-free personal care products on the skin.
- Avoid alcohol or other chemicals that are drying or irritating to the skin.
Lifestyle
Lifestyle recommendations include:
- Avoid those foods that are known to suppress immune function including: sugar, processed food, alcohol.
- Avoid food intolerances
- Ensure you drink adequate water.
- Adequate sleep assists in the healing process.
Naturopathic Therapies
The prescribing of naturopathic therapies requires the guidance of a naturopathic doctor as it depends on a number of factors including the causal factors, a person's age, prescription medications, other conditions and symptoms and overall health. It is always advisable to work with a naturopathic doctor prior to taking any natural therapies.
Naturopathic Therapies for boils or furuncles include:
- Clinical Nutritional Supplementation includes
- Vitamins such as Vitamin A, Vitamin C, Vitamin D, Vitamin E
- Minerals such as Selenium, Zinc, Copper
- Other supplements such as Flax Seed Oil, Essential Fatty Acids, Evening Primrose Oil, Quercetin and other Bioflavonoids
- Herbs either taken internally or used as herbal compresses include: Burdock (Arctium lappa), Calendula (Calendula officinalis), Slippery Elm (Ulmus rubra),
[9], Myrrh (Commiphora myrrha), Tea Tree Oil (Melaleuca alternifolia) [10], Hops (Humulus lupulus), Devil's Claw (Harpagophytum procumbens)[11], Aloe (Aloe vera)[12]
- Homeopathic remedies such as Tarentula, Calc Sulph, Hepar sulph
References
Reviewed by Iva Lloyd, BScH, RPE, ND [1]
- ↑ 1.0 1.1 Campbell James, Chapman Shane, Dinulos James, Zug Kathryn (2005) Skin Disease, Diagnosis and Treatment, Second Edition Elsevier Mosby
- ↑ 2.0 2.1 2.2 2.3 2.4 Stenstrom R, Grafstein E, Romney M, Fahimi J, Harris D, Hunte G, Innes G, Christenson J (Sept 2009) Prevalence of and risk factors for methicillin-resistant Staphylococcus aureus skin and soft tissue infection in a Canadian emergency department. CJEM;11(5):430-8. PMID:19788787
- ↑ 3.0 3.1 Murray Michael, Pizzorno Joseph (1998) Encyclopedia of Natural Medicine. 2nd ed. Three Rivers Press, New York
- ↑ Ridder-Schröter R, Marx A, Beer M, Tappe D, Kreth HW, Girschick HJ (2008) Abscess-forming lymphadenopathy and osteomyelitis in children with Bartonella henselae infection. J Med Microbiol;57(4):519-24. PMID:18349375
- ↑ Faden H, Lesse AJ, Trask J, Hill JA, Hess DJ, Dryja D, Lee YH (2010) Importance of colonization site in the current epidemic of staphylococcal skin abscesses. Pediatrics;125(3):618-24. PMID:20156893.
- ↑ 6.0 6.1 Parchman ML, Munoz A (2009) Risk factors for methicillin-resistant Staphylococcal aureus skin and soft tissue infections presenting in primary care: a South Texas Ambulatory Research Network (STARNet) study. J Am Board Fam Med;22(4):375-9 PMID:19587251
- ↑ 7.0 7.1 7.2 El-Gilany AH, Fathy H (Jan 2009) Risk factors of recurrent furunculosis. Dermatol Online J.;15(1):16. PMID: 19281721.
- ↑ Atanaskova N, Tomecki KJ (Jul 2010) Innovative management of recurrent furunculosis. Dermatol Clin.;28(3):479-87. PMID: 20510758.
- ↑ Engels Gayle (2008) Calendula HerbalGram.;77:1-2 American Botanical Council.
- ↑ Engels Gayle, Brinckmann Josef (2012) Myrrh HerbalGram.;93:1-4. American Botanical Council.
- ↑ Wegener Trankred (2000) Devil's Claw: From African Traditional Remedy to Modern Analgesic and Antiinflammatory HerbalGram.; 50:47-54 American Botanical Council.
- ↑ Engels Gayle (2010) Aloe HerbalGram.;87:1-5. American Botanical Council.