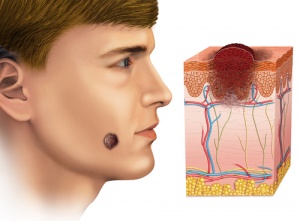
Melanoma
Melanoma develops via malignant transformation of melanocytes. It is the 5th most common cancer in men, and 7th most common cancer in women. Lifetime risk of developing melatonin is about 2% in both sexes. Melanoma is more common in fair skinned individuals, and is more prevalent in countries with higher percentage Caucasian populations.[1]
| Causes | Sunlight, Tanning beds, Family history |
|---|---|
| See Also | Women's Health, Oncology |
| Books | Books on Women's Health, Books on Oncology |
| Articles | Articles on Women's Health, Articles on Oncology (Cancer) |
| Article | "Night Shift Work Decreases Risk of Melanoma", NMJ, [1], 2011 October |
|---|
| Article | Photosensitizing Herbs for Skin Diseases and Cancer , 2011 May NDNR |
|---|
Contents
Naturopathic Assessment
Causal Factors
In order to stimulate the innate ability of the body to heal the causes of disease must be identified and addressed. Factors associated with melanoma include:
External
- Sunlight
- Intermittent sun exposure, commonly associated with holiday or weekend only tanning, increases the risk for melanoma. Chronic sun exposure, common in outdoor occupations, decreases risk of melanoma.[2]
- Tanning Beds
- There is a significant amount of evidence linking tanning beds to melanoma. Risks increases the earlier first exposure occurs.[2]
- Pesticide Exposure
- Pesticide exposure is correlated with increased risk of melanoma.[3]
Genetics
- Family History
- Individuals with first degree relatives with a history of melanoma are at an increases risk of developing melanoma themselves.[2]
- Phenotype
- Individuals with light skin colour, light eye colour, and skin that freckles easily are at increased risk of developing melanoma.[2]
- Genetic Risk
- There are several versions of genes encoding for pigmentation, DNA repair, and cell cycle regulation that confer risk for the development of melanoma.[2]
Physiology
- Melanocytic Nevi
- Those with a higher number of moles, or having dysplastic nevi, increases the risk factor for melanoma.[2]
Diagnostic Tests
Skin examinations performed by healthcare practitioners are an important aspect of early detection. The “ABCDE” criteria are used to evaluate suspicious lesions. ABCDE stands for:[1]
- A - Asymmetry – Early malignant melanoma lesions grow irregularly, and unlike benign pigmented lesions which are normally round and symmetric.
- B - Border Irregularity- Malignant melanomas tend to have irregular borders due to their uneven growth rate, unlike the regular margins seen in benign lesions.
- C - Colour variegation- Melanomas tend to contain several colours composed of combinations of tan, brown, black, red and white, while benign lesions tend to be uniformed.
- D - Malignant melanomas are generally over 6mm when diagnosed.
E- Evolution- Any change in shape, size, itching, bleeding, or pigmentation elevates suspicion of malignancy.
- Biopsy
- Skin biopsy remains the standard for confirming a diagnosis of melanoma. Excision, shave, and punch biopsies are all commonly used, with excisional biopsy being the preferred technique.[1]
- Staging
- Staging is performed based on histology, including tumour thickness, ulceration, and rate of division, as well as presence or absence of metastasis and lymph node involvement.[1]
Characteristics
Common Symptoms
Common signs and symptoms of melanoma include:[3]
- Painful Skin Lesion
- Changes in Skin Colour
- Suspicious lesion as defined by ABCDE criteria
Naturopathic Treatment Strategy
The goal of naturopathic treatment is to support and work in tandem with the healing power of the body. A treatment strategy is the most effective when it addresses the underlying causal factors and when it follows the naturopathic therapeutic order. The treatment strategy for melanoma is first prevention, followed by treatments to address the cancer directly or to support conventional treatments and to improve overall quality of life.
It is always advisable to work with a naturopathic doctor before engaging in any treatment plan.
Prevention
Prevention involves addressing any of the causal factors before they cause melanoma, including:
- Sun exposure behavior – modifying sun exposure, including limiting exposure to midday sun, and minimizing the risk of sun burns is recommended. The use of sunscreen remains debatable in prevention, as it does not entirely block UVB rays and may give individuals a false sense of protection.[2]
- Screening – screening is an important part of minimizing morbidity and mortality.[2]
Cancer Specific Treatments
| Article | Supplemental Vitamin A May Reduce Risk of Melanoma, 2012 August Natural Medicine [2] |
|---|
Follow the general guidelines for cancer specific treatments. Additional treatments that are specific to gastric cancer include:
- Dietary recommendations include:[3]
- Dietary Fat
- Reduction in fat intake is associated with a lower incidence of precancerous lesions in at risk individuals. Adherence to a Mediterranean diet has been shown to reduce the incidence of melanoma.
- Supplementation including:[4]
- Vitamins such as: Vitamin A, Beta-carotene, Vitamin C, Vitamin E, Vitamin D
- Minerals such as: Calcium
- Amino Acids such as: L-Cysteine
- Food Supplements such as: Fish oil, Melatonin, Green Tea, Indole-3-Carbinol, Modified Citrus Pectin, Selenium, Coenzyme Q10
Herbs such as:[3] Ginseng (Panax ginseng), Turmeric (Curcuma longa) Japanese Thuja (Thuja standishii)
Supportive Care
Follow the general guidelines for supportive care especially when conventional treatments such as surgery or radiation therapy are chosen.
References
- ↑ 1.0 1.1 1.2 1.3 Tuong W, Cheng LS, Armstrong AW (2012) Melanoma: Epidemiology, Diagnosis, Treatment, and Outcomes Dermatologic Clinics 30(1)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Berwick M, Erdei E, Hay J (2009) Melanoma Epidemiology and Public Health Dermatologic Clinics 27(2)
- ↑ 3.0 3.1 3.2 3.3 Najm WI (2012) Rakel: Integrative Medicine 3rd ed Chap 79 Skin Cancer Saunders
- ↑ Prousky J (2008) Principles and Practices of Naturopathic Clinical Nutrition CCNM Press